ARTUR FEDOROWSKI, M.D, Ph.D., ANDRZEJ STECIWKO, M.D, Ph.D. and JERZY RABCZYNSKI, M.D, Ph.D
ABSTRACT
Objective:
The influence of low-frequency electromagnetic (LF-EM) waves on the processes of carcinogenesis and tumor growth has been the subject of experimental investigations for more than two decades and the results are promising. In parallel, an interesting method of complementary medicine, biophysical-information therapy (BIT) or bioresonance therapy (BRT), which in principle is based on LF-EM stimulation, has emerged. BRT has been known since the late 1980s but is still poorly studied. The idea of applying BRT to tumors is based on two main premises: (1) endogenous biophotonic emission in the case of tumors is different from that produced by healthy tissues/cells and (2) BRT effects are believed to be primarily manifested at the immune-system level. Consequently, we decided to study the influence of BRT on a dynamic and well-known process: the expansion of transplantable hepatoma in rats.
Design:
The study was carried out on female Buffalo rats with implanted Morris tumors (three experimental and one control group). Fourteen (14) consecutive in vivo exposures using a BRT device (BICOM B 15, REGUMED Regulative Medizintechnik Gmbh, Graefelfing, Germany), were made from the third day after inoculation of the tumors. Biometric observations, intra vitam (tumor volume, growth ratio), were completed with histologic investigation (implantation locus, selected internal organs [lungs]).
Results: Thirty-one
(31) cases (69%; 11 = 45) of total tumor regression were observed in experimental groups and these individuals were anesthetized to enable histologic verification to be made. No lung metastases—usually observed in tumor-bearers could be detected. Moreover, in the inoculation loci, traces of former implantation and tumor absorption were found to be associated with high activity of cell-mediated immune response. No regressions were observed in the control group.
Conclusions:
We cannot exclude the possibility that LF-EM signals transmitted via BRT into the tumor-bearers may stimulate two separate processes: effective immunological response and/or tumor-cell death. The method appears to be capable of inducing the regression of transplantable hepatoma in vivo, thus is a potential subject of further studies.
INTRODUCTION
The influence of low-frequency electromagnetic (LFEM) waves on the processes of carcinogenesis and tumor growth has been the subject of numerous studies for more than two decades. These studies have concentrated on two main fields: estimation of risk factors related to the presence of artificially generated EM fields in our environment and a potential application of EM waves in the therapy of neoplastic states (Adey, 1993; Basset, 1995; Blank and Goodman, 1999; Goodman and Blank, 2002; Hong, 1995; U.S. National Academy of Sciences/National Research Council, 1996; Williams et al., 2001). The latter field involves various projects in which the electromagnetic spectrum is explored in the search for new methods allowing the inhibition of neoplasm expansion. There exists a parallel stream in the realm of complementary medicine called biophysical-information therapy (BIT) or bioresonance therapy (BRT), in which LF-EM stimulation plays a dominant role (Brugemann et al., 1993; Ludwig, 1995). The EM field is generated technically or modulated after detection, using generally the same methods as in the case of electrocardiograms (ECG) or electroencephalograms (EEG) (Ludwig, 1996). In principle, the applied spectrum does not exceed 150 kHz. Several electronic models have been designed since the late 1980s, but the fundamental elements remain the same: a detection system providing EM signals for the central unit in which modulation and/or generation takes place and finally an applicator system for the projection of EM waves upon the biologic object. The object (i.e., the patient) is usually connected to the output and the input at the same time, applicators being placed on various body parts (e.g., limbs). Until now, the BRT method has been poorly studied, which has resulted in a great gap between its proponents claims and the available experimental data.
The idea of applying BRT to tumors is based on two main premises. First, it has been proved that endogenous, biophotonic emission in the case of tumors is different from that produced by healthy tissues/cells (Popp et al., 1996; Van Vijk and Van Aken, 1991; Van Vijk and Van Aken, 1992). Although the examined spectrum corresponds to the optical frequencies, the existence of a similar phenomenon in the low-frequency band cannot be excluded. However, its detection encounters significant technical problems, for instance, thermal noise (Smith, 1995). The presence of endogenous, “biophoton-like” EM signals, originating from mutated structures (tumor cells) in the spectrum covered by BRT is only hypothetical. But if true, it can play a crucial role in either modifying the tumor-bearer’s response or even in directly inhibiting tumor growth. Second, according to some reports, BRT can act on the immune-system level (Kohler, 1997), and thus its stimulation may facilitate the processes of tumor-cell recognition and finally elimination.
In our previous experiments concerning the influence of BRT on transplantable hepatoma, the isolated tumor tissue was subjected to BRT prior to homogenization and inoculation in Buffalo rats. Injected animals, however, were not treated after the homogenate inoculation. The result was an acceleration of tumor growth (Fedorowski et al., 1997, 1998). In this paper, the effects of in vivo exposure for 14 consecutive days after tumor implantation are presented.
MATERIALS AND METHODS
Materials
Animals. The study was carried out on Buffalo rats (Animal Laboratory of the Department of Pathological Anatomy,
Wroclaw Medical University, Wroclaw, Poland); females, 4 months of age, body mass 210.0 g ± 15.0 g. The animals were housed in plastic cages with a wooden-shavings liner. The cages were placed in ventilated and illuminated accommodation at room temperature (approximately 22°C). The animals were maintained on a diet consisting of standard laboratory granules and water ad libitum.
Tumor. Morris hepatoma 5123D maintained by a serial passage in the Animal Laboratory of the Department of Pathological Anatomy (see above) was the object of the study. Morris hepatoma is a transplantable tumor coming from rat hepatocytes, primarily obtained by H.P. Morris, B.Sc., Ph.D., from the Department of Biochemistry, Howard University College of Medicine, Washington, D.C. The 5123 variant is moderately differentiated, grows locally, and produces early metastases to the lungs (Wepsic et al., 1976). According to a standard passage procedure, the tumor was excised from the tumor-bearer 3 weeks after implantation. All connective tissue and necrotic foci were removed. From the tumor sample, a homogenate was prepared under sterile conditions in a glass vessel.
Apparatus. A BICOM electronic device (version 4.1, model B 15, REGUMED Regulative Medizintechnik Gmbh, Graefelfing, Getinany) was used in the experiments. It was provided by a private owner. This electronic device is an example of an EM-wave modulator designed for BRT. It contains three basic elements: (1) input; (2) signal-processing circuits; and (3) output. The input signal (described as endogenous) is considered to originate from biologic objects that are placed in direct contact with the specially designed applicators. In this experiment, flat applicators with gold-plated brass on top were applied. They were insulated on the bottom by a cork layer, with a magnetic foil between the cork and the brass layer. The signal-processing circuits are made up of the following: optionally activated, components, (1) low- and high-pass filters that enable the transmitted band to be regulated in the ranges 10-1 kHz and 1-150 kHz, respectively; (2) phase inverter; (3) an absorption filter (patent-protected, molecular filter); (4) an amplifier/attenuator (range, 64-0.025 times); and (5) a system consisting of a wobbulator and a tuned band-pass filter characterized by a frequency range covering one octave around the fine-tuning frequency. This system enables the whole transmitted frequency band (10 Hz-150 kHz) to be swept in a predefined cyclic period (3-18 seconds).
The output signal (i.e., the input signal that was subjected to modulation and transmitted to the output) is emitted by an applicator identical to the input applicator and connected to the output of the device. Modulation parameters can be programmed on the front panel.
Methods
Preparation. The trial profile is presented in Figure 1. The tumor homogenate (dose volume, 0.3 mL) was implanted intramuscularly under sterile conditions in the form of an injection into the left femoral region in all experimental animals. Because of technical limitations, it was not possible to place a rat on the input and on the output applicator at the same time, which is otherwise possible in humans.
LF-EM LEADING TO MOR::SPATOMA REGRESSION
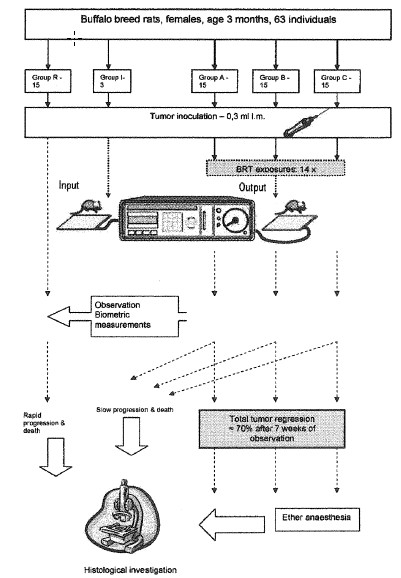
A, B, and C—There were experimental groups that were injected initially with Morris tumor, treated with bioresonance therapy (BRT) from the third till the eighteenth day and observed for 63 days. Those in which no palpable tumor was detectable were subsequently anaesthetized and histologic investigations were performed. Those who did not survive were classified as slow progression and final histologic investigations were performed)
I—These comprised an “input group” injected with Morris tumor, placed on an input applicator during all BRT exposures from the third till the eighteenth day (i.e., untreated). In this group no systematic biometric observations were performed and presence of growing tumor was confirmed by palpation.
R—This was the control group. Controls were injected with Morris tumor, untreated, and observed until natural death (approximately 4-5 weeks). Final histological investigations were performed on the controls. Histologic investigation was carried out using cuttings from the following areas: (1) primary tumor locus and (2) lungs.
Consequently, we decided to apply the following model of EM stimulation: we randomly selected three animals to be placed in a plastic cage with the input applicator at the bottom during all experimental exposures, thus serving as the source of a “standard” input signal for all exposed animals (input group 1). They were implanted but not treated during the experiment. Sixty (60) female rats were divided into four equal groups (15 individuals each), three experimental (A, B, C), and one control (R).
Exposure. As mentioned above, the source of the endogenous EM field for the BRT was the injected rats (input group 1). The signal to the BRT was thus dependent on the progress of the tumor development, imitating conditions during BRT in humans (where the input and output electrodes are placed on the same organism). We assumed that the EM field generated by a rat with an implanted tumor comprises both physiologic and pathologic components. The former are the result of the normal activity of organs and systems and the latter are the result of tumor progression and inflammatory processes in the host. The hypothetic goal of the treatment was to attenuate or extinguish pathologic components by applying phase inversion of the whole input signal (mode Ai, according to BRT). As a result, the target animals would receive the endogenous EM in the antiphase.
The exposures were realized in the range 10 Hz-150 kHz, which corresponds to the tuned band-pass filter range in the BICOM device (see Materials). This frequency band is believed to contain the most important endogenous EM signals (Brugemann, 1993). The filter was sweeping the whole spectrum from 10 Hz to 150 kHz and back for a period of 3 seconds, which was followed by a 1-second pause. The shortest possible sweeping period was chosen, because the bioresonance literature recommends it for dynamic, pathologic states (e.g., acute inflammation, as in the case of tumor growth). It is believed that such short-duration impulses do not interfere negatively with the physiologic functions of the recipient, who may promptly and positively react when pathologic components are extinguished (Brugemann, 1993; Ludwig 1995).
The amplitude of the endogenous signal was amplified 64 times (group A) or alternatively 8 times (group B). Group C was exposed to combined parameters A plus B. The maximal amplification (64 times) was chosen in order to attenuate efficiently the hypothetical pathologic components. However, we decided to apply even 8-times amplification in order to check whether a lower amplification grade would affect the result. The exposure time was set at 15 minutes (i.e. maximally), granted that the implanted tumor might require a higher dose to be inhibited. The choice of these exposure parameters was also supported by our previous studies and some available reports (Lakiza et al., 1995; Sakharov et al., 1995).
EM stimulation was carried out daily for a total of 14 days, beginning with day 3 until day 18 after implantation (except for two Sundays, i.e., days 9 and 16). The animals from groups A-C were placed in a plastic cage (3 at a time) with the output applicator at the bottom, in a respective order.
The summary of exposure parameters is presented below:
- Group A: Mode Ai (all frequencies, phase inversion on), tuned band-pass filter on, sweeping time 3 seconds, amplification 64 times, exposure time 15 minutes.
- Group B: As above except for amplification (8 times).
- Group C: Combined parameters for groups A and B (i.e., amplification 64 times) 15 minutes, and then amplification 8 times, 15 minutes (total time: 2 X 15 minutes).
Observation/Biometrical and Histologic Examination. Because Morris hepatoma is a solid tumor and grows locally, the tumor volume (V) can be estimated intra vitam according to the following formula V = 1 X w2/2, where 1 = vertical length and w = horizontal width. Because measurements of small tumors give unreliable results, we began our measurements of the tumor volumes on the eleventh day with approximately 3 days between the measurements. It was originally planned to survey the tumor growth until the natural death of the animals. This procedure allows the survival time and average growth ratio (GR) to be determined according to the formula: GR (g/day) final tumor mass ex vivo/survival time. However, the observation period was finally limited to 63 days (9 weeks), because many cases of total tumor regression were noticed in all experimental groups and this period corresponded to double the average survival time of the unexposed, tumor-bearing rats (i.e., the control group in this experiment). Animals that did not survive the observation period were investigated postmortem. The tumor was excised, measured, and saved for histologic examination, as well as whole lungs. Lung specimens were preserved, because Morris hepatoma metastasises mainly to this organ. Paraffin cuttings were prepared according to the following rule: (1) tumor cuttings from central and peripheral zones and (2) lung cuttings from all the lobes along the axis: (lung apex-lower lobe basis).
On the 63rd day, all animals that had survived the observation period and biometrically demonstrated complete tumor regression were anesthetized with ether. The thorax was opened and a blood sample from the left ventricle was collected for biochemical investigation (not reported in this paper). Amputated, left hind-limbs with the implantation locus were saved for further histologic investigation that included the examination of paraffin cuttings from central and peripheral zones round implantation locus. Lungs were treated as described above.
All the specimens were stained with hematoxylin-eosin (H&E). Morphologic estimation was carried out using a JeNaval microscope (Carl Zeiss Jena GmbH, Jena, Germany) and the picture-analysis program Multi Scan version 5.10 (Computer Scanning Systems, Warsaw, Poland). The person who examined the specimens was not informed regarding which group the specimens came from. It was, however, marked whether cuttings came from the tumor sites or lungs.
Statistical Analysis. Statistical analysis was performed, using Statgraphics Plus 6.0 for DOS software (Manugistics, Inc. Rockville, MD). The hypothesis of two means equality was applied (TWOSAM procedure) with estimation of the significance level (regarding p < 0.05 as significant). The mean value and standard deviation were calculated for each value.
RESULTS
From the eleventh day after inoculation, a substantial difference in the tumor-growth dynamics between the control and all the experimental groups was observed (Table 1). The tumor-growth rate was significantly reduced in the exposed groups, in which two alternative phenomena could be distinguished as the observation proceeded:
1. Gradual tumor regression after the initial period of slow progression with a critical date between days 17 and 21.
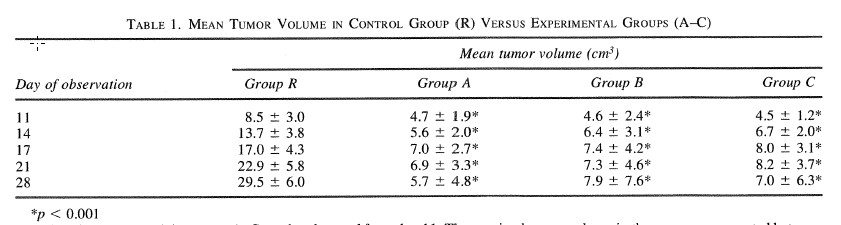
Reduced tumor growth in groups A-C can be observed from day 11. The maximal tumor volume in these groups was noted between days 17 and 21, whereas controls demonstrated steady progression.
LF-EM LEADING TO MO S HEPATOMA REGRESSION
Tumor Growth dynamics – day 21
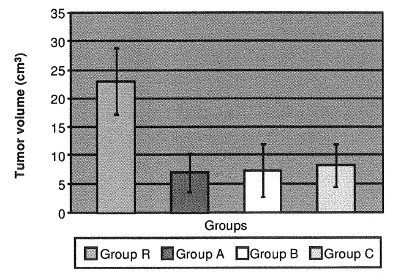
FIG. 2. Tumor growth dynamics on day 21. Increasing tumor volume differences, with time, between controls and exposed animals were observed. No significant differences among groups A, B, and C were demonstrated. R is control group.
From this date onwards, the regression processes predominated, resulting in a total decay of the palpable tumor.
2. Tumor-growth deceleration associated with longer survival time, compared to control group (slow-growing tumor).
The regression phenomenon predominated in the study. A total of 31 regression cases could be reported giving an approximate regression ratio of approximately 70% (highest in group C 80%). This process, however, made tumor measurements difficult and gave unreliable results, which became apparent from the 28th day. It was actually no longer possible to secure consistent biometrical data in the experimental groups. Nevertheless, the available data show a retarded tumor growth in exposed animals from day 11 until day 28, as can be seen in Table 1. The tumor-growth dynamics are also presented in Figure 2.
It is worth mentioning that no significant difference was observed between the mean tumor volumes when the three experimental groups A-C were compared.
We also decided to compare the tumor-growth dynamics in the rats with complete regression and in the rats with slow tumor progression, in order to identify the point of time at which the two subgroups began to show differences as regarded growth rates. Table 2 presents the biometric results after retrospective identification of the two groups. As can be seen, the point at which we could observe differences in growth rates occurred between days 14 and 17. It was completely manifested after the final BRT treatment on the 18th day. We also determined the growth ratio and the survival time in the slow-progression and control groups. In Figure 3, it can be seen that reduced growth ratio in the experimental subgroup was associated with increased survival time (56.7 ± 6.9 versus 38.7 ± 6.5 days, p < 0,001).
Histology
The histologic analysis revealed two different pictures of pathological changes in accordance with the above-mentioned division into two subgroups. They are discussed separately.
Slow progression. During the tumor investigation hepatoma tissue with a high mitotic activity was observed, in some cuttings with a presence of vast, coagulative necrosis and calcification foci (Fig. 4). Cross-sections revealed necrotic changes ranging from 25%-67% of the section area.
In lung cuttings metastatic changes in various stages of advancement were observed, from micrometastases and arteries filled with embolic material of cancer cells (Fig. 5) to macrometastases localised near the main bronchi.
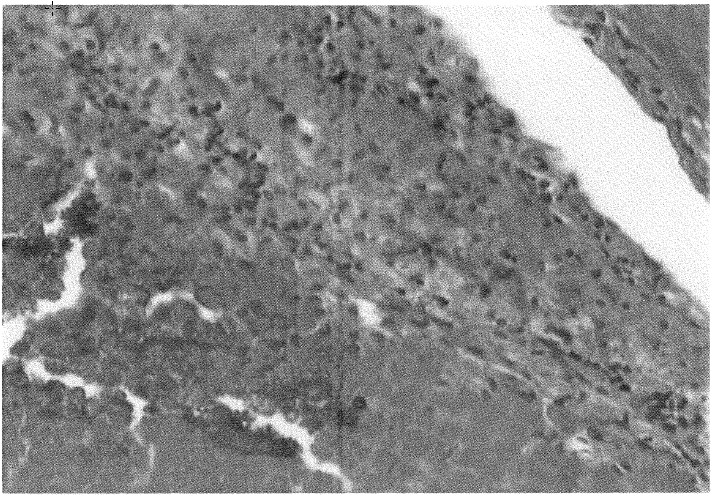
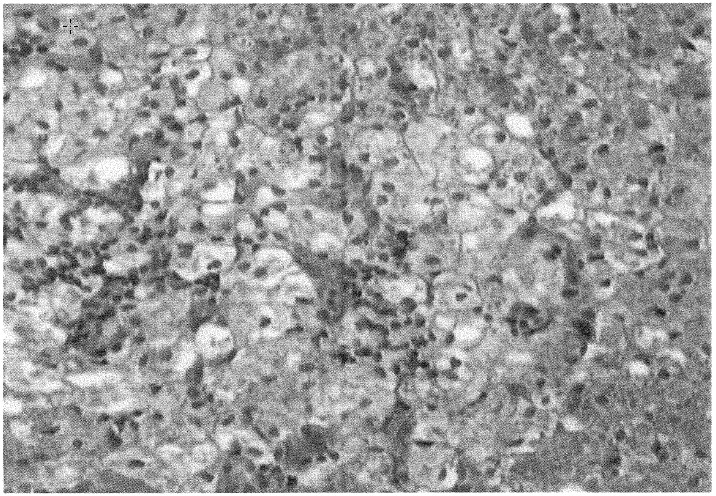
Regression. In the inoculation loci, traces of former homogenate implantation and tumor absorption were found: (1) resorptive granulomas, (2) hemosiderine deposits, and (3) intensive, inflammatory process with presence of macrophages and foam cells (Fig. 6). In several cuttings, nests of entirely or almost entirely necrotically transformed, hepatoma cells were observed, surrounded by macrophages and giant-cell embankment, granulocytic and foam-cell infiltration, hemosiderine deposits, and calcification foci (Figs. 7 and 8).

The group with manifested regression and the group with slow progression were compared. The results from the untreated control group are also shown.
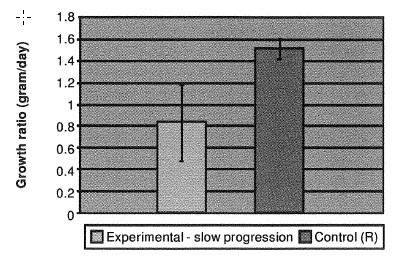
It must be emphasized that no lung metastases were observed in any lung section.
LISCUSSION
For many years, there have been discussions about the question of EM interactions with the living matter, according to the equilibrium-thermodynamics paradigm. That is, low-frequency EM fields have been considered too weak to bring about changes in the biological systems. In the last two decades, however, many studies have shown that non-thermal interactions actually can have biologic effects (Adey, 1993; Bistolfi, 1991). It is believed that the observed effects may be connected with unique quantum states and resonance responses in the biomolecular systems (Smith, 1994). Low frequencies (< 300 Hz) have been found to evoke various effects (e.g., altered enzyme activity or elevated transcript levels for specific genes; Blank and Goodman, 1999; Goodman and Blank, 2002; Hong, 1995). The threshold values for these effects seem to be extremely low. Blank reported that a magnetic field of 0.2-0.3 ,u,T might considerably influence the activity of selected enzymes (sodium, potassium — adenosine triphosphatase [ATDasel, cytochrome C oxidase) (Blank, 1997).
In parallel, some authors have raised the question of the therapeutic and biomedical application of EM fields (Basset, 1995; Sisken and Walker, 1995). Several in vivo studies show that exposure to LF, magnetic field (1 Hz to 1 kHz) may increase the survival time of tumor-bearing animals (Bellossi and Desplaces, 1991; Rannug et al., 1993). Other authors report direct cytotoxic (Jordan et al., 1996), immunostimulating (House et al., 1996) or antiangiogenetic effects (Williams et al., 2001). In light of these data, there seems to exist an integrative, biophysical field, which cre-
ates the basis for understanding the bioresonance principle.
![FIG. 4. Extensive coagulative necrosis and single calcification foci in tumor implanted in femoral muscle (hematoxylin and eosin [H&E], 120X).](https://bioresonance.org/wp-content/uploads/2016/04/low-frequency-electromagnetic-stimulation-may-lead-to-regression-of-morris-hepatoma-in-buffalo-rats-5.jpg)
![FIG. 5. Rat lung. Arterial vessel with metastatic hepatoma cells emboli (hematoxylin and eosin [H&E], 240X).](https://bioresonance.org/wp-content/uploads/2016/04/low-frequency-electromagnetic-stimulation-may-lead-to-regression-of-morris-hepatoma-in-buffalo-rats-4.jpg)
![FIG. 6. Implantation locus. Resorptive granulomas and hemosiderine deposits. No trace of intact hepatoma cells can be found (hema¬toxylin and eosin [H&E], 120X).](https://bioresonance.org/wp-content/uploads/2016/04/low-frequency-electromagnetic-stimulation-may-lead-to-regression-of-morris-hepatoma-in-buffalo-rats-3.jpg)
Undoubtedly, the therapeutic potential of BRT has not been sufficiently investigated to date. The aim of our study was to investigate the influence of BRT on a dynamic and well-known process—transplantable tumor expansion—in controlled laboratory conditions.
We were able to demonstrate that LF-EM stimulation according to the BRT model might inhibit tumor growth and finally even lead to total tumor regression. No significant difference was observed between two distinct amplifications (64X and 8 X ), but the combined exposure (64X + 8x) showed the highest regression rate (80%). It is unclear which factors are of importance for the initiation of the regression process and why some tumors proved to be resistant, although inhibited growth was observed as a result of the BRT treatment (slow progression).
There are a number of reports describing the influence of various factors on the dynamics of Morris tumor growth. Terlikowski et al. (1996) reported that local administration of tumor-necrosis factor-a (TNF-a)–recombinant could lead to growth inhibition and longer survival time. Other authors have observed the effects of various dietary components. However, no regression has been reported, only reduction of the gram per day parameter (GR) (Millis et al., 1996; Xu et al., 1996).
In our study, histologic investigation in the regression subgroup did not show any form of metastatic processes in the lung tissue, the prime target for metastatic cells. It is possible that either the tumor had been efficiently separated by the defense system or that the metastatic foci were gradually eliminated. It is worth mentioning that the immune system of tumor-bearing rats is subject to functional changes leading to the attenuation of cell-mediated response (Shevchuk et al., 1996). When the implantation loci were studied, it was noted that cell-mediated immunologic response (infiltration of macrophages, giant cells, and granulocytes, as well as intensive calcification and fibrosis) was evident and effective.
Consequently, LF-EM signals transmitted via BRT to the tumor-bearers seem to stimulate two separate processes: (1) effective immunologic response and/or (2) the death of tumor cells. The latter may take the form of either apoptosis or necrosis. At the present stage, it is, however, not possible to point to the right alternative. According to a quantitative model, weaker stimuli would trigger a limited release of lysosomal enzymes to the cytoplasm, followed by apoptotic death, whereas stronger stimuli would lead to a generalized, lysosomal rupture and rapid, cellular necrosis (Brunk et al., 1997).
Finally, we have to come to the crucial question. If we assume that the BRT device detects ultraweak, endogenous (but according to the biophotonic theory, coherent in nature), EM vibrations in the LF range, modulates them, and generates EM stimuli, what are the potential targets in the body?
Three hypotheses can be presented ad hoc:
- The endogenous EM field may comprise physiologic and pathologic components (e.g., originating from healthy tissues but also from tumors under expansion). Source and target are the same, and the direct action occurs on the basis of resonance phenomenon.
- Detected EM vibrations can constitute a source of additional stimulation of the immune system on the level of the hypothetical system of electromagnetic bioinformation (i.e., biophotonic, modulated in the lower range). This may lead to activation of tumor recognition and elimination.
- The modulated EM field is able to stimulate various systemic reactions, including the neurohormonal axis, and this can increase immune efficiency. This process requires the existence of electromagnetic couplings that reach beyond cellular and even systemic limits.
This work is only a modest attempt to try to find the answers to these questions. However, its results provoke more questions that one day may open up an entirely new avenue in contemporary medicine, integrating complementary and classic methods.
To conclude, LF-EM stimulation according to the BRT model appears capable of inducing the in vivo regression of transplantable hepatoma and may be a potential subject of further studies, including immunologic surveys.
ACKNOWLEDGMENTS
The authors would like to thank the staff at the Animal Laboratory, Department of Pathological Anatomy, Wroclaw Medical University, for their contribution, and Peter Engfeldt, M.D., Ph.D., Department of Clinical Medicine, Family Medicine Research Centre, Orebro University, for helping with the final editing of this manuscript. This study was partially supported by grant Number 683 from Wroclaw Medical University.
REFERENCES
Adey WR. Biological effects of electromagnetic fields. J Cell Biochem 1993;51:410-416
Basset CAL. Bioelectromagnetics in the service of medicine. Adv Chem 1995;250:261-76.
Bellossi A, Desplaces A. Effect of 9mT pulsed magnetic field on C3H/Bi female mice with mammary carcinoma A: Comparison between 12Hz and 460Hz frequencies. In Vivo 1991;1:30-40.
Bistolfi F. Biostructures and Radiation: Order Disorder. Turin: Edizioni Minerva Medica, 1991
Blank M, Goodman R. Electromagnetic fields may act directly on DNA. J Cell Biochem 1999;15:369-374.
Blank M. Biological mechanisms for electric and magnetic field interaction. In: Matthes R, Bernhardt JH, Repacholi MH, eds. Biological Effects of Static and ELF Electric and Magnetic Fields. Proceedings, International Seminar on Biological Effects of Static and ELF Electric and Magnetic Fields and Related Health Risks. Bologna, June 4-5, 1997. 1997:77-87.
Brugemann H, ed. Bioresonance and Multiresonance Therapy (BRT). Brussels: Haug International, 1993.
Brunk UT, Dalen H, Roberg K, Hellquist HB. Photo-oxidative disruption of lysosomal membranes causes apoptosis of cultured human fibroblasts. Free Radic Biol Med 1997;23:616-626.
Fedorowski A, Steciwko A, Rabczynski J. Influence of low-frequency electromagnetic field generated by transformation of endogenous Morris hepatoma field on its growth and metastatic ability (I). Med Sci Mon 1997;3:336-341.
Fedorowski A, Steciwko A, Rabczynski J. Influence of low-frequency electromagnetic field on growth of endogenous Morris hepatoma and its metastatic ability (II). Med Sci Mon 1998;4:765-773.
Goodman R, Blank M. Insights into electromagnetic interaction mechanisms. J Cell Phys 2002;192:16-22.
Hong FT. Magnetic field effects on biomolecules, cells and organisms. Biosystems 1995;36:187-229.
House RV, Ratajczak HV, Gauger JR, Johnson TR, Thomas PT, McCormick DL. Immune function and host defence in rodents exposed to 60Hz magnetic fields. Fundam Appl Toxicol 1996;34:228-239.
Jordan A, Wust P, Scholz R, Tesche B, Fahling H, Mitrovics T, Vogl T, Cervos-Navarro J, Felix R. Cellular uptake of magnetic fluid particles and their effects on human adenocarcinoma cells exposed to AC magnetic fields in vitro. Int J Hyperthermia 1996;12:705-722.
Kohler B. BiophysikalischeInformations-Therapie. Ulm: Gustav Fischer Verlag, 1997.
Lakiza 0, Lednyiczky G, Zhalko-Tytarenko 0. Cytotoxic effect of proper electromagnetic field on melanoma B16 cell culture. BEMS 17th Annual Meeting, Boston, June 18-22, 1995.
Ludwig W. The bioresonance therapy and the environmental factors from the physical perspective. Erfahrungsheilkuncb 1996;3: 168-170.
Ludwig W. SIT-System Information Therapy: Schwingungs-medizin in Theorie und Praxis. Spita Fachbuch Reihe, 1995.
Millis RM, Diya CA, Reynolds ME. Growth inhibition of subcutanously transplanted hepatomas by alterations of the dietary arginine methionine balance. Nutr Cancer 1996;25:317-327.
Popp FA, Li KH, Mei WP, eds. Recent Advances in Biophotons Research and its Applications. Singapore: World Scientific, 1996.
Rannug A, Holmberg B, Ekstrom T, Mild HK. Rat liver foci study on coexposure with 50Hz magnetic fields and known carcinogens. Bioelectromagnetics 1993;14:17-27.
Sakharov D, Savtsova Z, Lednyiczky G. Bioresonance therapy corrects the immunodeficiency of Chernobyl mice. BEMS 17th Annual Meeting, Boston, June 18-22, 1995.
Shevchuk LD, Baracos VE, Field CJ. Reduced splenocyte metabolism and immune function in rats implanted with the Morris Hepatoma 7777. Metabolism 1996;45:848-855.
Sisken BF, Walker J. Therapeutic aspects of electromagnetic fields for soft-tissue healing. Adv Chem 1995;250:277-286.
Smith CW. Biological effects of weak electromagnetic fields. In: Ho MW, ed. Bioelectrodynamics and Biocommunication. Singapore: World Scientific, 1994:81-107.
Smith CW. Measurements of the electromagnetic fields generated by biological systems. Neural Network World 1995;5:819-829.
Terlikowski S, Nowak HF, Lotocki W. Dynamics and phases of changes in the primary focus of Morris hepatoma under local application of cytokine hrec TNF-alpha. Neoplasma 1996;43: 125-132.
U.S. National Academy of Sciences/National Research Council. Possible Health Effects of Exposure to Residential Electric and Magnetic Fields. Official Report, October 31, 1996.
Van Vijk R, Van Aken H. Light-induced photon emission by rat hepatocytes and hepatoma cells. Cell Biophys 1991;18:15-29. Van Vijk R, Van Aken JM. Photon emission in tumor biology. Ex-perientia 1992;48:1092-1102.
Wepsic HT, Nickel R, Alaimo J. Characterization of growth properties and demonstration of tumor-specific transplantation antigens of Morris hepatomas. Cancer Res 1976;36:246-250.
Williams CD, Markov MS, Hardman WE, Cameron IL. Therapeutic electromagnetic field effects on angiogenesis and tumor growth. Anticancer Res 2001;21:3887-3891.
Xu G, Salen G, Lea M, Tint GS, Nguyen LB, Batta AK, Chen TS, Shefer S. Blocking late cholesterol biosynthesis inhibits the growth of transplanted Morris hepatomas (7288 CTC) in rats. Hepatology 1996;24:440-445.


